
How Is Medicare Changing In 2026?
Medicare evolves every year, and 2026 brings the first wave of negotiated Part D drug prices, updated premiums and deductibles, and expanded behavioral‑health and telehealth policies.
In this article, we break down what changed, why it matters, and the smart moves to consider before (and after) open enrollment windows.
Need one‑on‑one help reviewing your 2026 options? Senior Allies can walk you through it. Call 833‑801‑7999 for personalized guidance.
Calculate Your Medicare Costs Today
Create a Medicare action plan by estimating your total monthly premiums for healthcare and related expenses in retirement.
Get My Worksheet
1. Medicare Part B Premium and Deductible Increases
For 2026, Medicare Part B costs are rising again.
The standard monthly Part B premium will be $202.90. This applies to most Medicare beneficiaries unless your income is higher than average, in which case you may pay more due to IRMAA (Income-Related Monthly Adjustment Amount).
The Part B deductible is also going up by $26 to $283 in 2026. This means you'll need to pay this deductible before Original Medicare starts covering your healthcare costs.
2. New Part B IRMAA Chart
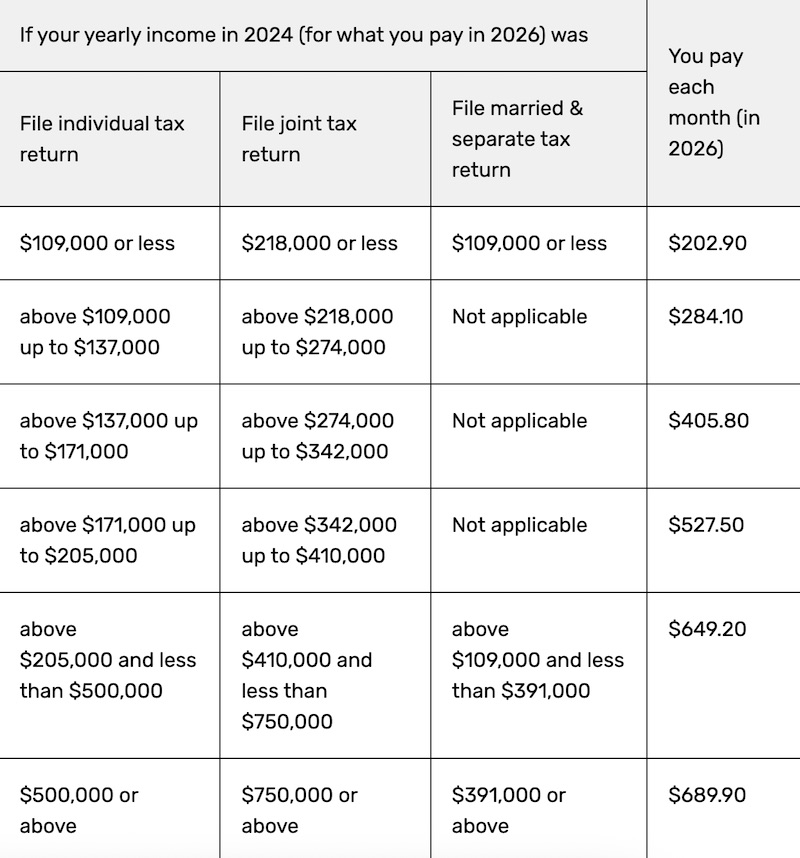
The standard Part B premium for 2026 is $202.90, but if your income is high, you'll have to pay more. This additional amount is known as the Income-Related Monthly Adjustment Amount (IRMAA).
Your IRMAA may vary depending on what kind of Part B coverage you have and how you file taxes. Below is an updated Part B IRMAA chart for 2026:
3. Medicare Part A Premium and Deductible Increases
Most people don’t have to pay a premium for Medicare Part A which covers inpatient hospitals, skilled nursing facilities, hospice, inpatient rehabilitation, and some home healthcare services. But if you fall within the 1% that does, that premium will be increasing in 2026, too.
In 2026, the Part A premium will increase to $311 (a $26 rise from 2025) for individuals with at least 30 quarters of coverage or those married to someone who does. For individuals with fewer than 30 quarters of coverage, and certain individuals with disabilities who have exhausted other entitlements, the premium will be $565 per month (a $47 increase from 2025).
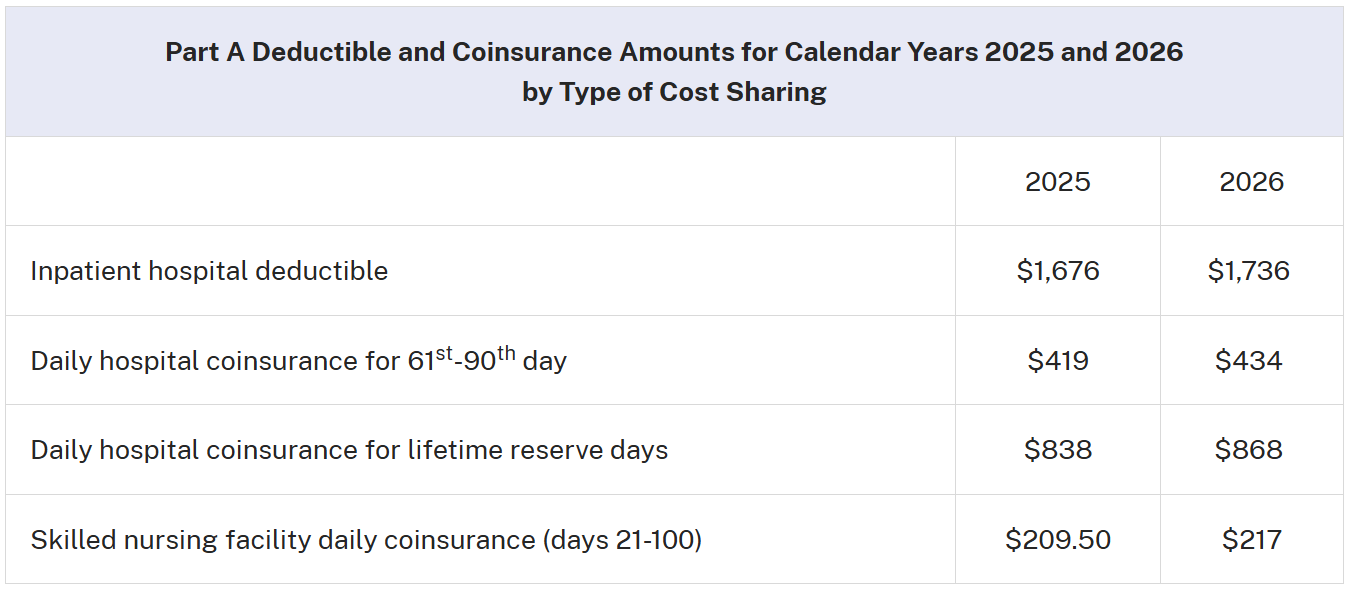
The coinsurance and deductible beneficiaries pay if admitted to the hospital are also going up a bit in 2026. Check out the chart below for the updated prices:
4. Lower Drug Prices Begin in 2026 as Negotiations Continue
As part of the Inflation Reduction Act, Medicare is continuing its multi-year process of negotiating prices for certain high-cost prescription drugs.
The first 10 drugs selected for negotiation already have their new, lower prices finalized, and those prices will take effect on January 1, 2026.
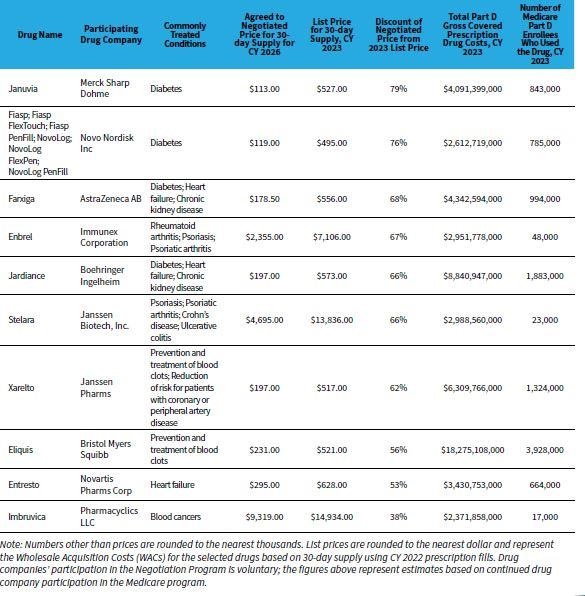
CMS also completed negotiations in 2025 for another 15 Part D drugs that were selected for the second cycle of the negotiation program. The new prices for this second group will take effect in 2027.
In 2026, Medicare will begin the third round of negotiations. CMS will announce up to 15 additional medications by February 1, 2026, and the negotiated prices for this group will take effect in 2028.
These ongoing negotiations are part of a broader effort to reduce out-of-pocket costs for Medicare beneficiaries, especially for people who rely on expensive, commonly used medications.
5. Changes to Mental Health Coverage & Telehealth
Through January 30, 2026, Medicare covers most telehealth services from anywhere in the U.S., including your home.
But beginning January 31, 2026, most telehealth services will only be available if you live in a rural area and receive the service from an office or medical facility located in a rural area.
However, even if you do not live in a rural area, you can still get certain telehealth mental health services from home after January 31. These include:
- Services for the diagnosis, evaluation, or treatment of a mental or behavioral health disorder, including substance use disorders
- Monthly End-Stage Renal Disease (ESRD) visits for home dialysis
- Services for the diagnosis, evaluation, or treatment of symptoms of an acute stroke
It’s also worth noting that Medicare Advantage Plans and some providers in Original Medicare may continue offering additional telehealth benefits beyond the standard rules. If your provider participates in an Accountable Care Organization (ACO), they may offer expanded telehealth options, too.
6. Updates to Caregiver Support
In 2025, Medicare rolled out caregiver training services to help caregivers learn how to give medicine, help with daily tasks, and better care for you at home. These trainings will continue in 2026.
Through January 30, 2026, caregivers can receive these training services through telehealth from anywhere in the United States.
Starting January 31, 2026, caregivers must live in a rural area and go to an office or medical facility that’s also in a rural area to receive these services through telehealth.
7. Coverage for Certain GLP-1 Weight-Loss Drugs in 2026
For the first time ever, beginning mid-2026, Medicare will start covering certain GLP-1 weight loss drugs used for weight loss. Up until now, these drugs could be covered for conditions like heart disease or stroke risk, but never for weight loss on its own.
This new pilot program will not be open to everyone. It is designed for about 10% of Medicare enrollees who meet specific criteria:
- Severe obesity (a BMI over 35)
- A BMI over 27 with prediabetes or established cardiovascular disease
- Obesity along with advanced kidney disease, heart failure, or uncontrolled high blood pressure
This new coverage will be offered through Medicare Part D prescription drug plans.
Until the pilot program launches in 2026, here’s what Medicare currently covers:
- Medicare Part B covers obesity screenings and behavioral therapy for beneficiaries with a BMI of 30 or higher.
- Medicare Part D may cover GLP-1 medications, but only when they are prescribed for diabetes or another approved condition.
- Medicare does not cover weight-loss drugs when they are prescribed solely for losing weight.
Additionally, if you do not qualify for the Medicare pilot program or if your insurance does not cover GLP-1 medications, a new government website called TrumpRx.gov is set to launch in January 2026.
This program will allow anyone to buy certain GLP-1 medications at a reduced price — starting at about $350 per month — regardless of insurance status.
8. New Mid-Year Benefits Statement Begins in 2026
Starting in 2026, Medicare beneficiaries will begin receiving a Mid-Year Benefits Statement, a new tool designed to help you understand what Medicare services you’ve already used — and what important benefits you may still be missing.
This statement will arrive sometime during the summer and will show:
- Preventive services you’ve already received
- Preventive services you haven’t used yet
- Any gaps in recommended screenings
- Personalized reminders about no-cost Medicare benefits
- Information on how to schedule the services you still need
The goal of this new statement is to make it easier for you to keep up with your health and avoid missing out on valuable benefits.
9. Part D Medicare Changes
Medicare Part D helps cover prescription drug costs, but some major changes are coming in 2026. Let's take a look at how these changes might affect your prescription drug coverage.
Fewer Part D Plans in 2026
For 2026, there will be a total of 360 stand-alone Prescription Drug Plans (PDPs) nationwide, which is a 22% decrease from 2025.
This means you may see fewer drug plan options in your state this year.
On the bright side, there are still many Medicare Advantage Plans with drug coverage (MA-PDs) available.
Even though the number of MA-PD plans has dipped slightly in the last two years due to changes in federal payments and shifts in healthcare costs, there are still around 21 Medicare Advantage prescription drug plans available in Macon County for 2026.
These Medicare Advantage drug plans often have lower — or even $0 — monthly premiums compared to stand-alone PDPs.
For some people, bundling medical and drug coverage together in an MA-PD plan may offer good value. We have a total of 14 MA-PD plan options here in Macon County for 2026.
If you’re unsure which type of plan makes the most sense for your situation, a Sams/Hockaday agent can help you compare your options.
Part D IRMAA Premiums Are Going Up
Individuals with higher incomes may pay a higher premium due to income-related adjustments. The table below shows these extra amounts for high-income beneficiaries.
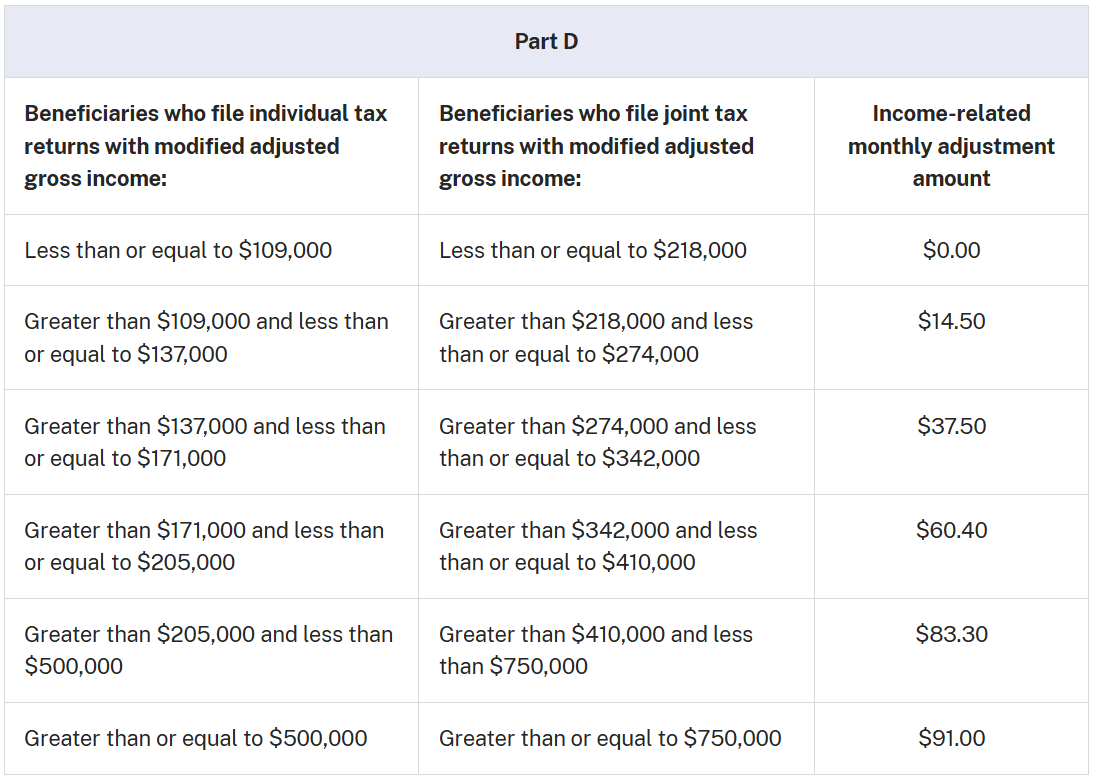
And for those who are married filing separately:

New Cap on Out-of-Pocket Drug Costs
In 2026, Medicare will cap your out-of-pocket drug costs at $2,100 per year. Once you reach this limit, you won’t have to pay anything for covered Part D drugs for the rest of the year.
If you're eligible for Extra Help, your costs may be lower or even covered.
Payment Plan Option for Prescription Drugs
Part D plans must continue offering the Medicare Prescription Payment Plan in 2026, which allows you to spread your out-of-pocket drug costs over the year instead of paying them all at once.
This program doesn’t reduce the cost of your medications, but it can make budgeting easier. If you choose this option in 2025 and stay in the same Part D plan, you’ll automatically be in the program for 2026.
Conclusion
Medicare is always making changes, so it's good to stay up-to-date on what's happening and make sure you understand how these changes will affect you.
If you have questions about how these updates may affect your coverage in 2026, give us a call at 217-423-8000.
A licensed Sams/Hockaday agent will be happy to walk you through your options and make sure you feel confident about your plan.
Get a Free Policy Review
Do you have the best plan with the best rate? Schedule a free policy review, and we'll help you compare all your options.
Review My Policy


